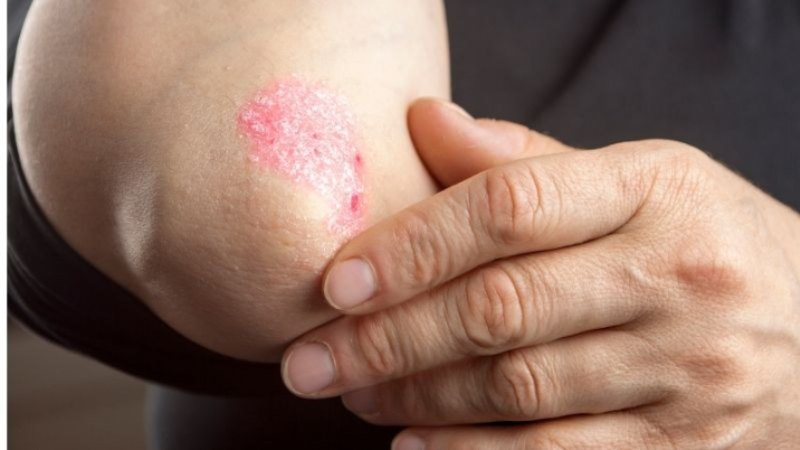
An autoimmune skin condition, psoriasis is typically identifiable by red and scaly patches that tend to be itchy. It’s a common skin disease that may affect anyone. The chronic nature of this condition means that there isn’t any cure for it. The intensity of the symptoms of psoriasis can vary from none to severe. There could be a time period, ranging from days to weeks to months, when the symptoms happen to be severe. Post this flareup, you may observe the severity decreasing and eventually symptoms going away. After some time has passed by, the symptoms could start manifesting again. If there haven’t been any active symptoms of psoriasis for a while, this time period could be considered as remission period. However, there remains a possibility that symptoms may show up again in the future.
Why psoriasis happens?
Even though the precise causes behind this disease may not have been pinpointed yet, there is some understanding regarding the vital factors which are at play here.
Basically, what causes psoriasis is the overly fast multiplication of the skin cells, which can possibly be attributed to issue with the immune system. Usually, the generating and shedding process of the skin cells takes place over a period of a month. But in the case of psoriasis, this timeline is reduced to a number of days only. Because the skin cells regenerate at an abnormal, rapid rate, as a result the cells begin to build up. Plaques, which are a pretty common symptom of psoriasis, are a result of this chain of events.
In addition to the immune system, genetics are considered an important factor too. However, it’s important to note that a person without any family history of psoriasis could also suffer from this condition.
Psoriasis is not a contagious condition, so one person can’t pass it on to others.
Potential factors that may trigger psoriasis symptoms
It’s important to keep in mind certain factors that could act as trigger for this skin disorder. The symptoms could manifest themselves or get aggravated as a result of these triggering factors.
Skin injury

If there has been any trauma to the skin, maybe a scrape, cut, bug bite, or any other kind of injury, then that may act as a possible trigger for psoriasis.
Cold weather

A psoriasis flareup may happen due to dry and cold climatic condition. In contrast, warm weather can help with psoriasis symptoms.
Stress

A common as well as key trigger of psoriasis is stress. The close corelation between excess of stress and psoriasis flareups means that it’s crucial to reduce stress in order to manage psoriasis more effectively. Living with psoriasis can be stressful in itself. Just remember that stress management will be beneficial for psoriasis management too. So, choose healthy ways to destress yourself.
Infections
Sometimes, psoriasis symptoms may be triggered by other infections that the immune system may be dealing with. For example, any skin infection, ear infection, strep throat, respiratory infection, etc could probably lead to a psoriasis flareup.
Certain medicines

Antimalarial medicines, lithium, medicine for high blood pressure, etc are a few kinds of medication that could act as triggers.
More trigger factors

Alcohol and smoking are some other likely triggers for psoriasis, and so are things like very dry skin, particular foods, and hormonal changes.
Since different people have different triggers for psoriasis, you’ll need to put in some time and work into discovering the specific triggers for your individual case. Maintain a diary where you note down each time there’s an instance of psoriasis flareup. Observe what factors could have contributed to this instance, what symptoms have occurred, and how serious are these symptoms. Over time, you may be able to interpret a pattern of the factors causing psoriasis flareups for you.
Here are some common symptoms of psoriasis
When it comes to psoriasis symptoms, each person is likely to have a different experience. The kind of psoriasis they’re affected by and the areas of body affected are a few important factors determining their experience. The following list can be considered as some common signs of psoriasis:
- Red colored patches covered by scales that look silvery and thick.
- Skin looking cracked and dry. There might be some itching or bleeding here.
- Stiffness and swelling in joints
- Plaques that feel itchy.
The patches/scales could exhibit anywhere on the body, but they can typically be found affecting areas like elbows, scalp, and knees. Some other body areas where these could exhibit are neck, hands, face, feet, and genital areas.
Different kinds of psoriasis
The five types of psoriasis are as follows:
Plaque Psoriasis
Present in nearly 80% of people having psoriasis, plaque psoriasis is the most common kind of this skin disorder. As the name indicates, this type is characterized by raised skin patches with plaques or scales over them. The usual areas where these plaques affect are elbows, scalp, back, knees, etc.
Pustular Psoriasis
This is a relatively rare kind of psoriasis, impacting around 3% of people having psoriasis condition. White bumps filled with non-infectious pus and red skin around these bumps is a common symptom of pustular psoriasis. With more prevalence in adults, the extent of pustular psoriasis could vary from being limited to certain areas to being spread across the body.
Guttate Psoriasis
Tiny, red-like bumps mark this type of psoriasis, which typically occurs in childhood. Infection like a strep throat is a common trigger of guttate psoriasis. Mostly, these bumps can be seen on the legs, arms, torso, but they can also affect the body elsewhere.
Erythrodermic Psoriasis
Erythrodermic psoriasis is a rare yet serious form of psoriasis which could even be life-threatening, which is why it’s imperative that medical care is sought urgently when it happens. The symptoms might appear pretty much all over the body, red rash along with severe burning or itching sensation.
Inverse Psoriasis
This psoriasis type shows itself in the form of patches that appear red and smooth. These can be found in the skin fold areas of the body. Examples of areas would include genital and groin regions, under breasts, abdominal folds, and armpits. Things like rubbing/friction and perspiration can make inverse psoriasis worse.
How to live with psoriasis?
The treatments for psoriasis are focused towards improving and managing the symptoms, and ensuring that the chances of developing related health issues are reduced. Moreover, it helps to adopt certain lifestyle practices that promote better quality life. Eating healthy, avoiding or reducing alcohol use, consciously staying away from triggering factors, and effectively minimizing any stress, are all good ideas when it comes to managing psoriasis.
Having a well-established emotional support system is essential. Therefore, it’s important for you to communicate with your close ones or even a professional, if necessary, about the challenges that you experience having psoriasis as a part of your life.
Follow Wat-Not on Facebook, Twitter, Instagram, and Pinterest.